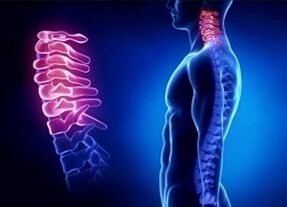
Secondary degree of osteocartilage degeneration in the cervical region supporting the pillar is a pathology faced by people of different ages.Many people ignore the initial stages of the disease, symptoms of degenerative and malnutritional processes and develop pain.
Doctors recommend paying attention to signs of osteochondrosis in the cervical vertebrae.Do not wait until the cartilage between the disks is damaged, which will cause the patient to continue to feel pain and violate the mobility of the neck.It is important to know that with the severity of discocardium pathology, brain hypoxia develops, dangerous brain diseases emerge, and the risk of ischemic stroke increases.
General information
The first degree of the disease is almost asymptomatic: sometimes there is pain in the neck, and you will feel a slight muscle tension in your palpation.If you start treatment in time: gymnastics, painkillers, cartilage protectors, vitamins, massage, then it's enough to stop the degeneration starting process.
In the absence of proper treatment, the disease progresses.Doctors in patients with headaches often detect the second degree of cervical bone cartilage in the spine, exerting unpleasant sensations when tilting and turning the head, limits of movement, muscle tension in the neck and shoulders.
Important points of osteochondrosis at 2 degrees in the cervical vertebrae area:
- A crack in the annulus appeared, and the instability of the cervical spine occurred.
- Crime during the spreading process (which ensures the full nutrition of the disc) adversely affects the condition of the cartilage tissue, while the destruction of important elements begins.Violating the amortized structure can cause lower disk height, vertebrae close to each other, and movements of the head and neck can cause pain.
- The pressure on the nerve roots increases and periodic pain occurs.They can be eliminated with painkillers, but the unpleasant feeling is quickly restored after the medication expires.
- In the second stage of the disease, the vertebral artery does not actively compress, but the patient feels other signs of pathology: lethargy, sleep disorders, increased fatigue, and decreased performance levels;
- With cervical bone-cartilage degeneration, the pain is not only locally in the problem area, but also spreads on the back of the head, upper back, and shoulders.The progression of the disease in the context of the innervation of the neighboring sector can lead to brain complications.
- In the absence of treatment, the negative factors are maintained, pathologically 3 degrees, and the active damage to the fibrous annulus and hyaluronic acid laying.The study was herniated and disc hernia, persistent pain during vertebrae friction, problems with cervical mobility, and bright neurological disorders.
Causes of pathological development
Osteochondrosis in the cervical region develops in the context of:
- Low temperature;
- Violation of posture;
- calcium deficiency and vitamins;
- The habit of sitting is to bend down and bow your head.
- Working on a computer for a long time;
- Genetic tendency;
- Cervical injury;
- Too much load on the neck area and too much head movement;
- Improper metabolism of minerals in various pathological backgrounds;
- Endocrine disease;
- The head is often abandoned in the process of performing professional responsibilities.
According to ICD -10 M42, Cervical Code Level 2 Osteochondrosis.
Symptoms of cervical osteochondrosis
Progress in cervical osteochondrosis suggests an increase in pain syndrome, worsening in the wellbore, unpleasant sensation in the upper back, especially after stress or staying in a position for a long time.The closer the vertebrae that moves to each other, the more aggressively the ligaments descend, and the muscle strains seem to maintain the optimal position of the support pillar.
The combination of subluxation of vertebrae and a reduction in the effects of the muscle frame enhances discomfort in the affected area.The displacement of elastic laying can promote neck turns, increasing pain when bending and extending.
The protrusion of the disk changes the correct position of adjacent bone structures, and an invasion of posture occurs.If you don't start treatment, continue with uncontrolled painkiller intake, you will soon experience negative symptoms of 3 degrees cervical bone cartilage.
diagnosis
The treatment was performed by a vertebral scientist.You can also contact a neurologist.
For diagnosis, profile experts illuminate clinical pictures and anatomy, prescribed X-rays from the cervical department and MRI.In the case of severe muscle spasms, electromyography is required, and if the patient complains of obvious brain disease, multiple blood vessels are required.
notes!After diagnosis, doctors often noticed that patients had a tertiary disease, but using tool studies can still identify positive progress in the process.If you do not start treatment in an emergency, then symptoms of vertebral artery compression are subsequently damaged in the brain circulation and the development of hypoxia in vital organs will soon be full of effort.
Effective therapeutic areas
After diagnosis, doctors recommend eliminating factors for disease progression.If degeneration stops - malnutrition changes in cartilage, the pathological process will soon affect the bone structure and blood vessels, and a set of negative characteristics will appear.Due to the severe pathological level, it is difficult to prevent the process of cartilage destruction, and damage to the annulus, doctors reveal the eruptions and hernia of the intervertebral disc.
drug
The doctor chose several sets of medications:
- Cartilage protector.The composition prevents the destruction of the slimming protein washer and activates the process of cartilage tissue regeneration.The course starts from 3 months.
- NSAID.Eliminates inflammation in the nerve roots, reduces pain and swelling, and improves mobility in the problem area.Drug Form: Transdermal Plaster, Capsule, Suspension, Tablet, Gel, Ointment.
- musorelaxant.They help painful muscle cramps, promote exercise, and relax muscle fibers.
- Vitamin B.Neurotic substances are essential to restore the transmission of nerve impulses when pinching sensitive structures in the process of osteochondrosis.
- Pain analgesics.For headaches, ordinary analgesics should be taken to deal with background discomfort in muscle tone and damage to the intervertebral disc.It is necessary to remember: painkillers will only reduce discomfort, but if osteochondrosis is not treated, unpleasant feelings of cervical spine, shoulders, headaches, brain diseases, it will be aggravated as orthopedic pathology progresses.
- sedative.Sleep disorders, headaches, and discomfort in the head can have a negative impact on the condition of the nervous system.The patient becomes irritable and has more insomnia.Helps with plant compounds and synthetic medicines: Desert tin agents, soothing plant plants, Walle-style tablets and tin agents based on roots, mint soup, lemon balm.
In most cases, 2-degree corticosteroids and drug obstruction are not required for intervertebral pathology: malnutrition and degeneration processes on the disc, adjacent tissues are less active to promote pain.Promote the status of these drug complexes.If the doctor is not opened, it is impossible to use powerful analgesics: have 2 degrees of illness and have sufficient preparation for moderate exposure.
Other treatment methods
Patients should remember: Use only drugs to stop the progression of cervical osteochondrosis.Complex treatments are prerequisites for restoring depreciation laying, reducing pain, eliminating muscle cramps, and normalizing neck mobility.
Effective method:
- Neck massage, including points;
- Use Lyapko and many of the largest Ipplitor Kuznetsov;
- Hirudtherapy;
- acupuncture;
- Physical Therapy: Ozokerric applications using effective analgesics and anti-inflammatory drugs, Mudlet, UHF, electrical and voice therapy;
- Physical therapy exercises and special exercises for cervical osteochondrosis;
- Manual therapy;
- Wearing a wooden stick collar.
Possible complications
Without timely complex treatments, osteocartilage will progress, brain dysfunction occurs in the context of vertebral artery compression, nerve root pinch.The longer a patient visits a neurologist or spondylosis doctor, the more aggressively the disc will be destroyed, and the risk of severe brain disease will increase.
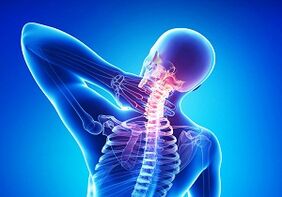
The progression of cervical osteochondrosis usually causes a variety of pathological and dangerous conditions:
- Cervical osteochondrosis and dizziness of nausea and fainting;
- ischemic stroke;
- Changes in the spine;
- A low-oriented cone was developed around the neck, commonly known as the "Widow of Hump";
- Pain syndrome in the neck area, nape.Changes in weather conditions, and head movement increases discomfort;
- Blood pressure jumps;
- herniation and a more dangerous form of pathology, rupture of the annulus, bright pain syndrome - hernia of the intervertebral disc;
- Severe headaches, including the nature of migraines;
- Numbness in the cervical area, shoulders, unpleasant tingling, pain and decreased sensitivity of the hands.
To prevent cervical osteochondrosis and prevent pathology from transitioning to a more severe 3-degree transition, patients must perform doctors’ prescriptions, take medications, do gymnastics for the neck, participate in massage therapy, and use transdermal patches to affect the problem area.It is important to give up smoking, eat correctly, not bend over, change head position more often during workdays, but avoid sudden movements.No treatment is required, irregularities in the procedure, reduction of cartilage protective agents, frequent pressure, hypothermia, and hypoarthria are factors that increase the risk of cervical osteochondral bone marrow disease.



















